Clinical trials frequently include multiple end points that mature at different times. The initial report, typically based on the primary end point, may be published when key planned co-primary or secondary analyses are not yet available. Clinical Trial Updates provide an opportunity to disseminate additional results from studies, published in JCO or elsewhere, for which the primary end point has already been reported.The primary analysis of the Early positron emission tomography (ePET) Response-Adapted Treatment in localized Hodgkin Lymphoma H10 Trial demonstrated that in ePET-negative patients, the risk of relapse increased when involved-node radiotherapy (INRT) was omitted and that in ePET-positive patients, switching from doxorubicin, bleomycin, vinblastine, and dacarbazine (ABVD) to bleomycin, etoposide, doxorubicin, cyclophosphamide, vincristine, procarbazine, and prednisone (BEACOPPesc) significantly improved 5-year progression-free survival (PFS). Here, we report the final results of a preplanned analysis at a 10-year follow-up. In the favorable (F) ePET-negative group, the 10-year PFS rates were 98.8% versus 85.4% (hazard ratio [HR], 13.2; 95% CI, 3.1 to 55.8; P value for noninferiority =.9735; difference test P <.0001) in favor of ABVD + INRT; in the unfavorable (U) ePET-negative group, the 10-year PFS rates were 91.4% and 86.5% (HR, 1.52; 95% CI, 0.84 to 2.75; P value for noninferiority =.8577; difference test P =.1628). In ePET-positive patients, the difference in terms of PFS between standard ABVD and intensified BEACOPPesc was no longer statistically significant (HR, 0.67; 95% CI, 0.37 to 1.20; P =.1777). In conclusion, the present long-term analysis confirms that in ePET-negative patients, the omission of INRT is associated with lower 10-year PFS. Instead, in ePET-positive patients, no significant difference between standard and experimental arms emerged although intensification with BEACOPPesc was safe, with no increase in late adverse events, namely, second malignancies.
Windows en Linux
Houdt de toets ctrl ingedrukt en draai het muiswiel omhoog of omlaag
Of houdt de toets ctrl ingedrukt en druk tegelijk op de toets + of -
Of ga rechtsboven naar instellingen en gebruik de instelling zoom
Mac
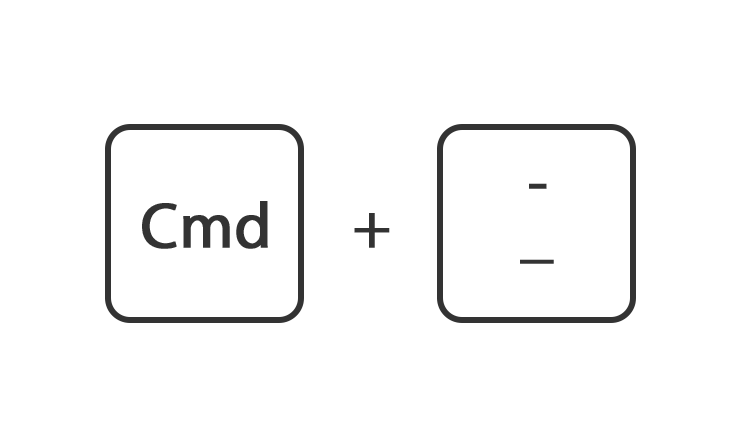
Houdt de toets command ingedrukt en druk op de toets + of -
Of ga rechtsboven naar instellingen en gebruik de instelling zoom.